That being said, we only promote authors, products, and services that we wholeheartedly stand by!

“AIP Stories of Recovery” is a success story series about regular people from the Autoimmune Protocol community who are changing their lives using the protocol. Each month a new person is featured and readers have the opportunity to discover all the different health challenges that are being overcome by folks just like themselves on the same path. At Autoimmune Paleo we hope you’ll be inspired by, empathize with, and learn from these stories. If you are interested in sharing your story, please email us through the contact form.
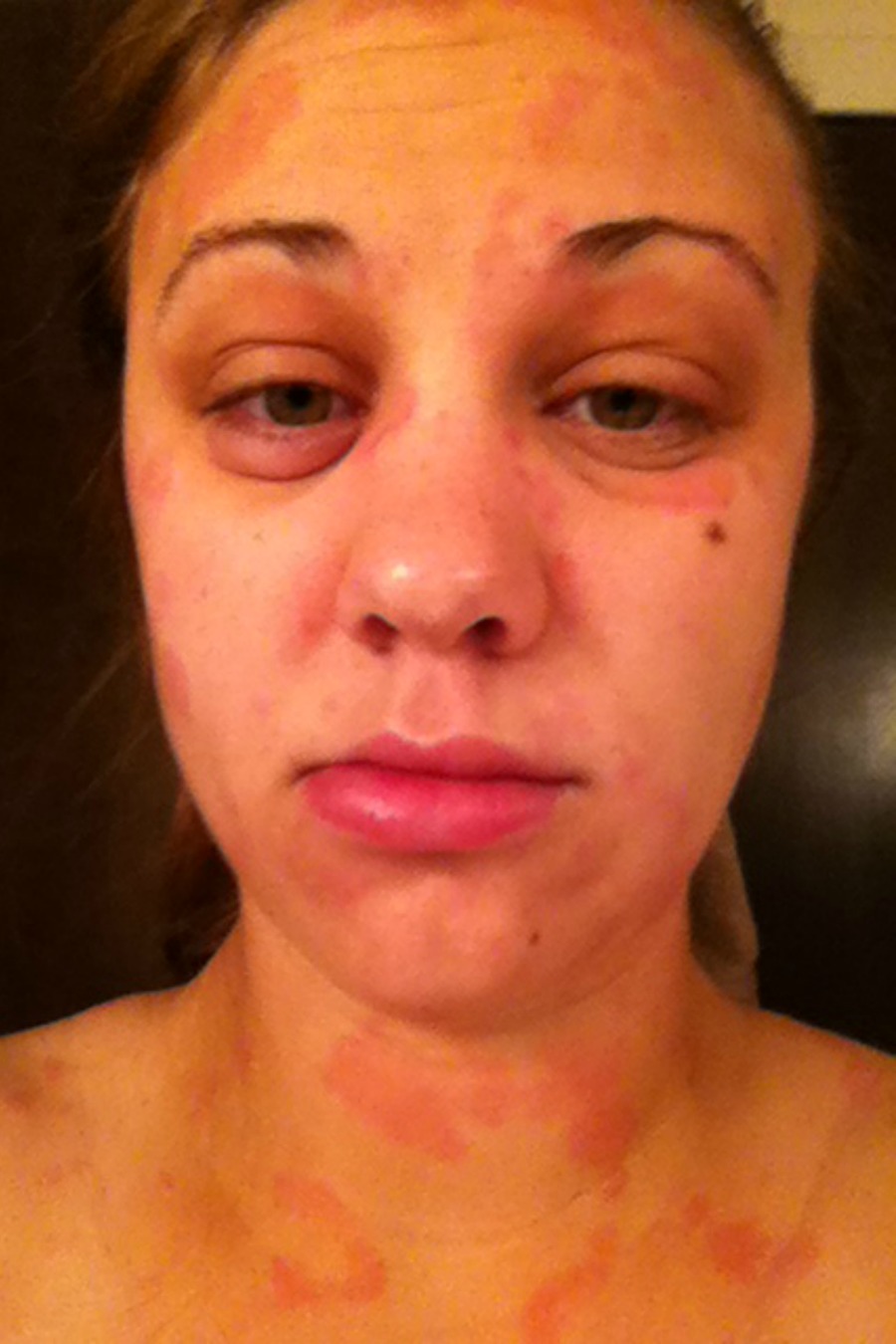
Meet Julie! Julie literally woke up with severe condition and spent months in pain and with no hope of it improving, despite taking huge doses of powerful drugs. Her primary AI is autoimmune-driven chronic idiopathic urticaria and angioedema , a condition that left her at times unrecognizable due to hives and swelling. Julie did not accept the answers handed to her by the conventional system though and instead used diet and lifestyle to overcome her health struggles. Her recovery is particularly dramatic, because it is visible.
What health issues are you dealing with, when did they begin, and how long did it take to get a diagnosis?
I woke up one morning in April 2013 (after having a high fever and stomach cramps the night before) and discovered red, itchy bumps on my knees. The next day they showed up on my arms, so I called my doctor. My original diagnosis was acute hives, thought to be an allergic reaction to the antibiotics I was taking for a sinus infection. I went on Prednisone and the hives went away, but flared up again after I tapered off the steroids. For the next six weeks, I went through a cycle of steroid bursts and hive flare-ups, with each flare-up worse than the last. I would wake up every morning with hives all over my body. The itch was so severe that it was painful and all consuming. No creams provided relief, nor did high daily doses of four different antihistamines.
In late May, I started to experience seemingly random swelling of my hands, feet, lips, and eyelids. I would also develop severe hives and swelling anywhere on my body that was subject to sustained friction (e.g., from backpack straps or my shoes). I had been an active person and was training for a triathlon, and one day my feet swelled so painfully after a run that I could barely walk without assistance. I missed a lot of work because I was too embarrassed to show my swollen, red face at the office. I went from being a healthy, active young woman to being afraid to go outside for a walk.
Finally, I saw an allergist/immunologist who diagnosed me with chronic idiopathic urticaria (hives) and angioedema (swelling). “Idiopathic” means that there is no apparent explanation. When I asked my doctor why this would suddenly start happening to me, his response was that I “might just be a hivey person.” I didn’t find this answer acceptable and started researching everything I could about my condition. I was desperate for answers. In the meantime, my doctor put me on a daily dose of Prednisone. The side effects of all the drugs were terrible – I had trouble sleeping because of the steroids, and when I finally did fall asleep, the high doses of antihistamines gave me nightmarish hallucinations. Eventually, in July, my test results led my doctor to conclude that my condition was “autoimmune-driven.” I was told it was possible I would have hives for years.
Describe what your lowest point with your health journey was like?
There is an injectable drug called Xolair that has been used for about a decade to treat asthma, and at the time was in the process of being evaluated by the FDA for treating chronic hives. Because it had not been approved at the time (it has since), my insurance company wouldn’t cover the drug, and its cost was prohibitively high – about $800 per shot. During one appointment with my immunologist, he told me they had an extra vial of Xolair “lying around” that they would administer to me. I was the last appointment of the day, however, so they told me to call later in the week to set a time to come in for the injection. When I called several days later, I was informed that the doctor had changed his mind and that giving me the Xolair was “not the best course of action.” I was completely and utterly heartbroken. At this point I was deeply depressed and realized that I had been hanging all of my hopes on this unattainable drug. I started to prepare myself mentally to have my condition for the rest of my life, but it seemed unbearable. I was terrified of the future, when I should have been excited – my husband and I had just bought our first house and I had a great job. But the daily pain consumed me and itching had become my new reality. I felt alone even though loved ones surrounded me.
What challenges influenced you to look for a solution? Basically, what was the tipping point?
The tipping point was probably the same as my low point. I decided that Western medicine was only going to continue to fail me and if I was going to get my life back, I had to take matters into my own hands. My years of eating a poor diet, not getting adequate sleep, working out too hard, and not managing my stress had caught up to me, and it was up to me to turn things around, start listening to my body, and give it what it needed to heal. This was in the fall, and I couldn’t even spend time outside in the cold without my face swelling to the point that I was unrecognizable. I refused to accept a life where I was afraid to go outside, a place that had always been restorative and inspiring to me. I refused to accept that I would have to take steroids for the rest of my life just to function. I decided to start seeing a naturopath and at about the same time was introduced to the Whole 30 and the Paleo diet by a coworker.
When you found a protocol to help you heal, what was it and what was your first indication that it was working?
I started my first Whole 30 on the Autoimmune Protocol in October 2013. I also took an ALCAT food sensitivity test at the recommendation of my naturopath, and the test confirmed that I had a moderate or severe sensitivity to foods prohibited on the AIP such as wheat, eggs, soy, and nightshade vegetables. Unfortunately, I also learned that there were some “safe” foods that I could not tolerate, such as beef and onions. It was a challenge at first, but I was ready to try anything. Within two weeks on this protocol, my “good days” began to get better and my “bad days” were not as bad. One morning I woke up with no hives, which hadn’t happened in months. I had my last ever bout of angioedema about two weeks into the 30 days. I eventually found that I could tolerate grains like corn, rice, and oats, and slowly started trying to reintroduce other foods. After a few months I could eat eggs again, but I still would have a flare of hives if I tried to eat nightshade vegetables or nuts/seeds. By early January 2014, my hives were so small I couldn’t even tell if they were really hives. By the end of January, I was in complete remission. I slowly began to taper off the steroids I had been on for six months and did not have a flare-up. By early May 2014, I was finally off steroids completely. In July, when tomatoes came into season in my area, I slowly added them back with success – a food I hadn’t enjoyed in nine months.
What resources have you used on your healing journey so far and how did you find them?
The first resource I was introduced to was the Whole 30 Website and the book It Starts With Food by Dallas and Melissa Hartwig. I searched “autoimmune paleo” online and discovered this blog. The recipes and words of support were an indispensable resource on my journey. I also found a wealth of information and recipes on Pinterest (search “AIP”) and still use it regularly. Finally, I stumbled across an online support group on Yahoo Groups for sufferers of chronic hives. This group helped me to feel less alone in my struggles, and I also discovered a protocol for a low-histamine diet, which provided relief for many in the group. I incorporated aspects of the low-histamine diet into my own protocol and found that it helped in my recovery.
Did your doctors suggest any treatments that you rejected and if so, why did you choose to try other methods?
My doctor did not suggest any treatments that I rejected, but he did reject my repeated assertions that my diet and lifestyle changes were responsible for my dramatic improvement. Despite this, my view has been permanently changed by my experience. I continue to avoid processed foods and gluten and limit nightshades; I listen to my body and try to take care of myself. Instead of covering up my symptoms with medication, I am now continually tweaking this holistic approach to improve my physical, mental, and spiritual health.
It can seem like our lives are consumed by a chronic illness, but there is so much beyond those struggles. What brings you true joy right now?
My experience with a chronic, debilitating illness taught me to truly savor and be grateful for the simple pleasures in life. Now, I feel true joy when I can take my dog for a walk and enjoy the fresh air and exercise without fear of pain and itching. I revel in the taste of nourishing foods that I know are making me healthier. And most of all, I look to the future with great optimism, instead of trepidation.
Want to learn more about how AIP works? This story shares one individual’s experience, but you can explore the broader evidence in our AIP medical research review and start with our Autoimmune Protocol guide.














20 comments
Wow! That’s just what i needed to read right now. I also have chronic hives and angiodema which I’ve had for 18 months. At first I went down the normal path and went through a couple of bouts of prednisone and lived on super strong antihistamines. I tried laser allergy therapy, acupuncture, food elimination and finally I found AIP and I think I’m starting to see the light at the end of the tunnel!! Hooray for AIP! I also recently got a food sensitivity test done and found out that beef, an AIP safe food is a no go for me. So thanks for this post, I’ve kept thinking I’d love to know if there’s anyone out there with the same issues that”s proved help doing this protocol. I too have some hideous photos of me on bad days and I totally get the staying home in embarrassment part. Ouch! I still am taking the weakest antihistamine I can find, sometimes every day, sometimes every other. My goal is to get off it completely. So, thanks for the incentive to keep going. It IS possible!
Adelle, I’m so sorry to hear that you are also struggling with hives and angioedema, but I’m glad that you seem to be finding some answers! I took a food sensitivity test as well and reacted to beef and other AIP-safe foods like onions and coconut. It was challenging to find ways around these limitations, but in the end 100% worth it. Have you looked into the low-histamine diet at all? It restricts high-histamine foods and also identifies other strategies like freezing leftover meat right away (histamine levels start to build if you leave it in the fridge). I found that diet protocol to be helpful as well.
Good luck and don’t lose hope!
I have had chronic idiopathic urticaria for at least 20 years and I just began AIP protocol to the best of my ability. I stay on a maintenance dose of Claritin, Pepcid and a small dose of lorazepam at night. I have so many allergies I can’t count them and every day they increase. I hope I can still recover at my age.
Bernadette, we’ve seen folks of all ages make progress on their health journeys. Sending you healing vibes and good luck for the road ahead.
Just found your site by way of searching food allergies /testing. I’ve had chronic allergies beginning at 6 months of age . Asthma ,eczema , hives 🙂 pollen, grass, ragweed, histamine reactive bad, dust, pet dander, and way to many foods to list. Dairy bloats me. Among many health problems . I started Paleo roughly 7 months ago, in hopes to find relief , With not a whole lot of luck . I found I’m not just allergic to nightshades , most cruciferous veg. vinegar , fermented foods , coconut products, many fruits . Maybe have a fructose problem there .
I’ve had to pick and choice which foods don’t bother my allergies as much – It’s maddening !! I’m really beginning to think it’s chemicals of some sort, but if I’m eating natural it shouldn’t be possible ? Lately I have seriously been thinking of doing the MRT- Leap allergy testing , but every thing I read about it – says it’s not accurate and misleading . So I’m feeling pretty lost any ideas would be welcome at this stage … Xcrossing Fingers – Looking for answers ?
Hi Diana,
I think you will find this article from one of our contributors, Eileen Laird very helpful: https://autoimmune-paleo.com/why-food-intolerance-testing-doesnt-work/
Wishing you the best!
I know this comment is late, but I just wanted to say, thank you for sharing your inspiring story, Julie. I don’t know WHAT is wrong with me, but my new doctor (this is #9, as the first 8 did not know how to help me!) has diagnosed my problem as being autoimmune. Among other things, I’ve had painful swelling above my eyes for over a year now – my eyes look similar to yours in the “before” picture. I can’t wear make-up anymore because it hurts my face, and I just hate going out in public. I’m so embarrassed of how I look. I have completed several Whole30s in the past year with no improvement, so now I am on AIP. I have also recently taken an ALCAT test and I am also intolerant to many AIP friendly foods (like COCONUT! Boo!). I’ve been really depressed about things lately so I was happy to come across your story tonight. Maybe there is hope for me.
Jane,
Just popping in to say I am so happy you found it helpful, and we are all wishing you success on your recovery. Take care!
Hi Julie – I have to say that as I read this my heart both raced and ached at the same time. I have struggled with the exact same AI condition as you since 1993 and can literally feel your pain (and itching). My story, like yours was one filled with desperation and frustration (you can read about it here: https://jessicabeacom.com/my-real-food-journey/) where at my lowest point I was pretty sure I couldn’t live another day in pain – everything so swollen I could hardly walk, close my hands into fists or open my eyes. Antihistamines didn’t work for me, I refused to take immunosuppressants and after 12 years of nearly daily steroids I finally found a diet that worked for me. It Starts with Food was my savior and from there I found AIP. After a successful round of Whole 30 and a few months of AIP (and lots of other functional testing and tinkering with my diet) I’ve found a way to live nearly flare free for the better part of 3 years. When I do have a flare it’s usually brought on by a virus and easily treated with a steroid dose pack – so far I’ve averaged only 1-2 per year which is pretty amazing considering how advanced my condition had become.
I just wanted to thank you for sharing your story. As you can see, it really resonated with me and hit home. I applaud your work (and that other the other AIP bloggers here) because there are so many people out there living dark days with an AI condition and this is a place where they can find hope, encouragement, knowledge and empowerment to take back their health and their lives.
Thank you!! Much love!
Jessica
Wow…I have had several episodes of chronic hives, with all the problems and symptoms described in this article. I also had Grave’s Disease and I have psoriasis. I am just starting to read your information on this diet but it would be wonderful to be able to keep these problems under control without taking multiple medications.
Hi Kim,
So sorry to hear of your struggles, and wishing you a swift recovery!
I am also suffering from chronic hives and angioedema. It has been 6 months now and now my body is immune to anti-histamines and steroids. I am ready to start a holisitic approach for this terrible terrible condition! I have missed SO many days of work and can barely get out of bed from all the medicines, itching, and swelling. My doctor wants me to start on Xolair but it is so expensive, terrible side effects and can take months to start work. I would like to start this diet and also maybe a juice detox to begin. How did you start your journey? Should I meet with holisitic doctor first? I want to be sure it is okay to do with all the medication I am. Any tips, comments, and suggestions are welcome!
Hi Emily! Thanks for being here, and sorry to hear about your struggles. We do suggest meeting with your doctor to let them know about the elimination diet and if there is anything you should be aware of with your medications. We don’t suggest doing any detox program in conjunction with the elimination diet, it is pretty intense as it is! Wishing you luck!
Thank you. I read your story in tears today. I have been dealing with the same AI issues since October 2015 and I am having trouble making it. It is so hard to get through the day sometimes. I have a husband and three little girls, and I know that I am not able to be the mom and wife that I want to be right now. Today was the first time I had ready a story about someone going through the same thing as me. Thank you so much for sharing, and being so brave. You are an inspiration. I think there might just be hope for me yet.
I’ve been suffering with Chronic Idiopathic Urticaria for over 2 months now. I just recently started getting bouts of Angiodema, which are absolutely horrific. I’m only 24 years old! I’ve been taking antihistamines 2x a day for 2 months now, Zantac 2x a day, Singulair before bed, and now back on Prednisone because of how bad the hives/angiodema has been. It seems like all my primary doctor wants to do is prescribe drugs to suppress it for now but it’s obviously not getting down to the root cause. I had one appointment with a Naturopath and he ordered a IGG food antibody test which I haven’t got the results back yet, but hopefully find some answers there. I have a couple questions.. Did you stop taking the medications like antihistamines, steroids, etc when you started the AIP diet? If not, when did you stop taking them and how effective was it? I’m in such a rut… I want to start taking supplements and probiotics but I’m worried taking all these prescription drugs won’t make them effective at all? Help! I could use some answers. Thank you!
I am so glad I found this story! Everything that you said is what I have thought for the past year. I am going to start the AIP lifestyle change once the new year starts.
Hooray Cheyenne! Wishing you so much luck!
Hi there! Thank you so much for the information! I’m who being how long you were on AIP or whole 30 before you saw improvement. Also, did you eat low histamine at the same time or just adopt some of the principles, if so which ones? Thank you!
Lizzy
“Just a hivey person” sounds like my allergist. I’m glad I found this article I’ve been debating on doing the AIP diet for some time. I’ve previously had luck with Paleo but I stupidly went off the deep end and started eating all the things that made me feel awful to begin with i.e gluten and dairy and all the forbidden foods. Now I’m worse off than what I was previously and Paleo just isn’t cutting it nor are the occasional dose of antihistamines. Wish me luck on my journey *fingers crossed*
You got this, Tanya!