
While herbalism today is touted as a trendy alternative healthcare option, the study and practice of plant medicine for healing has been around since time immemorial. The first written records of medicinal plants appear on Sumerian clay tablets dated over 5,000 years old with archaeological evidence suggesting that medicinal plants have been used as far back as 60,000 years ago (The Herbal Academy, 2016). Until very recent history – as in, the last 100 years – herbal medicine was the primary method of healthcare used by all people, from midwives and folk healers to doctors in established medical institutions. Every culture around the world has its own relationship and frameworks for working with plants but they all agree on this: herbs are approachable, safe, and effective.
When it comes to autoimmune disease, however, things can get a bit confusing. We all know that autoimmune healing can be a difficult undertaking and that we are often presented with conflicting information from both the scientific community and our own bodies. What research came out last week might change in just a few months. What works one day for us may not the next. If we look at autoimmune healing from a traditional context, we can examine how herbalists and healers of old supported these conditions throughout history. This is what we refer to as empirical evidence. This historical information can be extremely empowering, especially as modern research around botanical interventions is often limited.
How can herbs be incorporated into the autoimmune protocol?
Herbs can be utilized to directly modulate an overactive immune system, to support secondary organ systems of the body that are being affected by autoimmunity, to palliate symptoms in acute times of illness, for deep vitamin/mineral/phytonutrient nourishment, and to help us with things like getting a good night’s sleep, soothing a bout of gas and bloating, easing sore joints/muscles, and so much more.
The practice of herbalism is vast and for me to discuss all the ways in which medicinal plants may be used to support autoimmune disease would require an entire book! Here I’ll attempt to answer some of the most common questions I get from clients in my practice and other practitioners who are interested in utilizing herbs but don’t know where to start.
What herbs are safe for autoimmune disease?
I wish I could answer this simply, but there are no hard and fast rules. Every person is unique and requires individualized care, especially when they have an autoimmune disease. What works for me may not work for you. That said, here are a few safety tips to keep in mind when exploring internal use of herbs:
Check for interactions. Herbs CAN be used in conjunction with over the counter and prescription medications, including drugs like LDN, levothyroxine, or immunosuppressants. It is imperative that you check for potential interactions whenever thinking about taking herbs. A qualified clinical herbalist, naturopath, or integrative doctor should be able to provide you with a list of herb-drug interactions. You can also often find some of this information online.
Stick to herbs with years of traditional use. Don’t fall for the hype of trendy superfoods and targeted advertisements. Some of the most “popular” medicinal plants we hear about in the media are often endangered plants, or are driven to at-risk status because of the media hype around them. Some of these plants do not have hundreds of years of traditional use, or they are subject to cultural appropriation, and oftentimes studies of botanicals focus on isolated constituents, are in vitro studies, or both. This gives us limited information on how these plants will actually affect people in practice. Basically, we don’t know what we don’t know. It is always safest to start with basic nutritive herbs that have been used for hundreds of years. For more information on at-risk plants to avoid, check out this list from United Plant Savers.
Trust your own body. Introduce herbs that may interact with the immune system in the same way that you would introduce a food during the reintroduction phase of the AIP diet. In my practice, I have seen a few clients with autoimmune diseases react to herbs like astragalus, while ten other people are totally fine with it and find benefit from incorporating it into their routine. Keep a symptom journal and test things out!
When in doubt, seek help. Clinical herbalists (sometimes referred to as medical herbalists in Canada and Europe) are specifically trained to be able to support individuals with complex medical conditions. Some naturopaths receive education on botanical medicine as do integrative/functional doctors, but not all are well versed in traditional & modern research around herbs. If you seek out a practitioner, ask them about their training and make sure they have experience with autoimmune conditions. I have seen well-meaning practitioners harm autoimmune sufferers because they didn’t understand the nature of these diseases – advocate for yourself just as you would with the rest of your medical team.
Immunostimulants vs. Immunomodulators
When researching herbs for autoimmune disease, you are going to see two words thrown around: immunostimulant and immunomodulant. These are considered to be herbal actions – keywords that describe the effects an herb will have on the body.
Immunostimulants, also known as “immune stimulants”, “immune enhancers”, or “immunopotentiators”, generally stimulate immune system activity. Immunostimulating herbs are typically used on a short-term basis at the onset and through the duration of an infectious illness. These are the herbs to use caution around if you have an autoimmune disease.
Immunomodulants, also known as “immune modulants”, may support our immune system’s ability to fight off pathogens while specifically reducing immune activity associated with autoimmune reactions and hypersensitivity (Agnelini, 2016). These are the herbs that herbalists often use to safely support clients with autoimmune diseases.
Below are two tables to help you identify which herbs are immunostimulants, which are immunomodulants, and some additional notes to keep in mind when working with these plants.
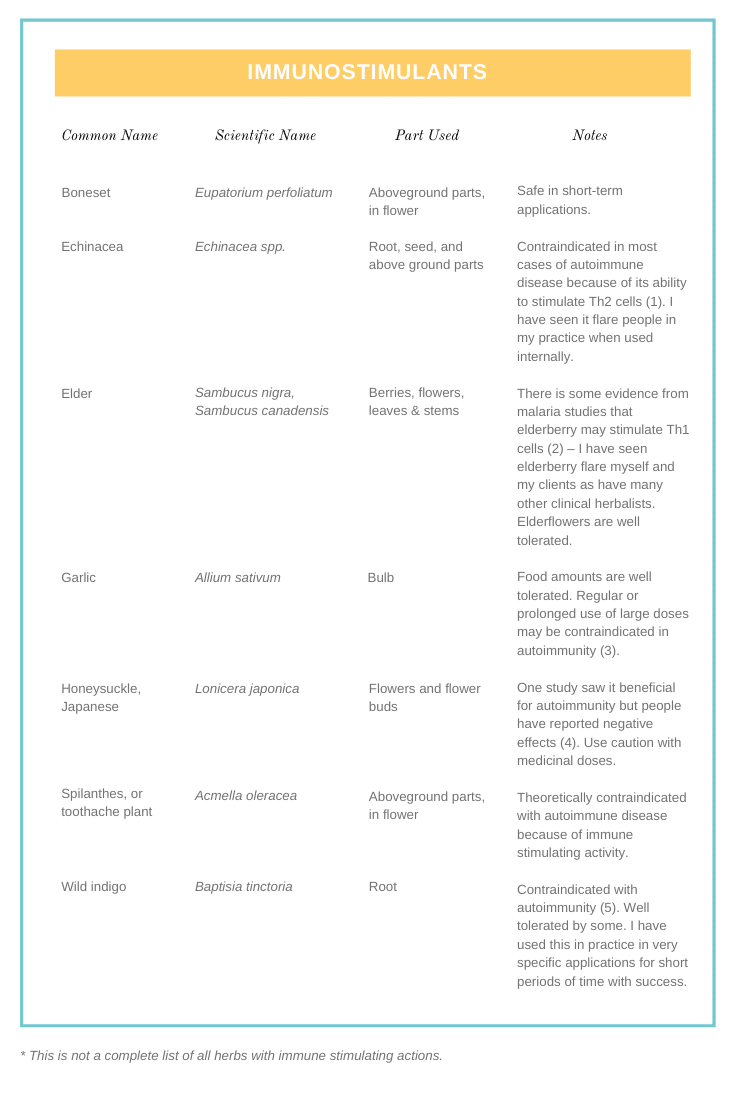
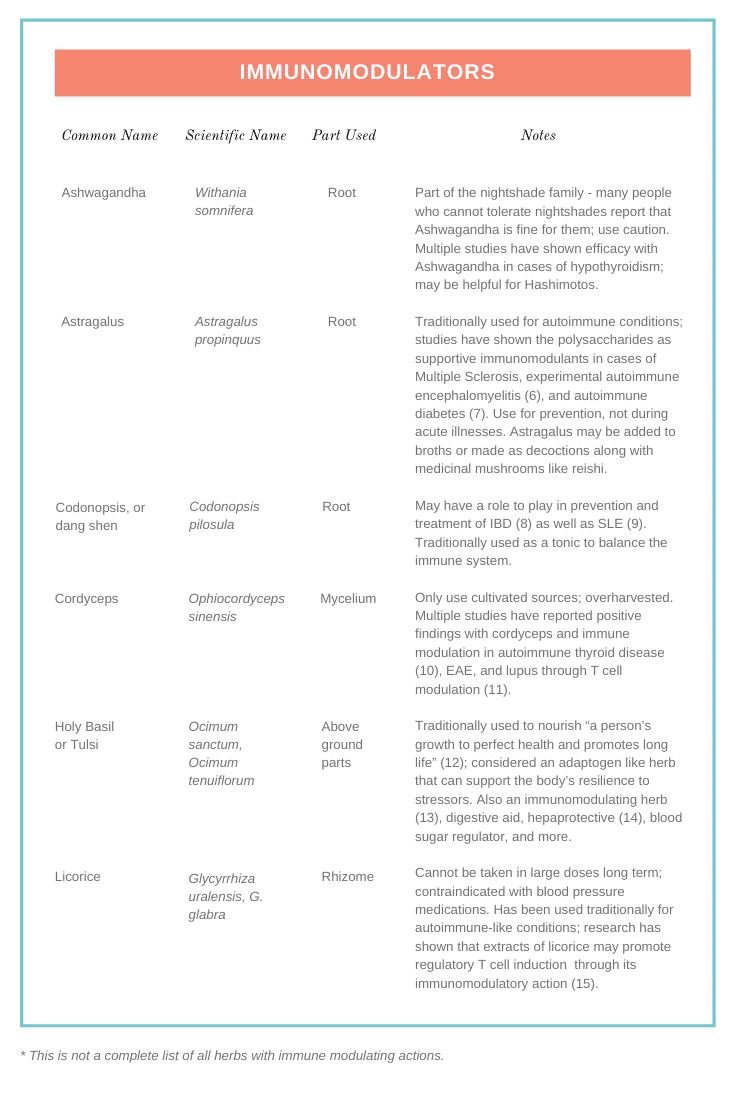
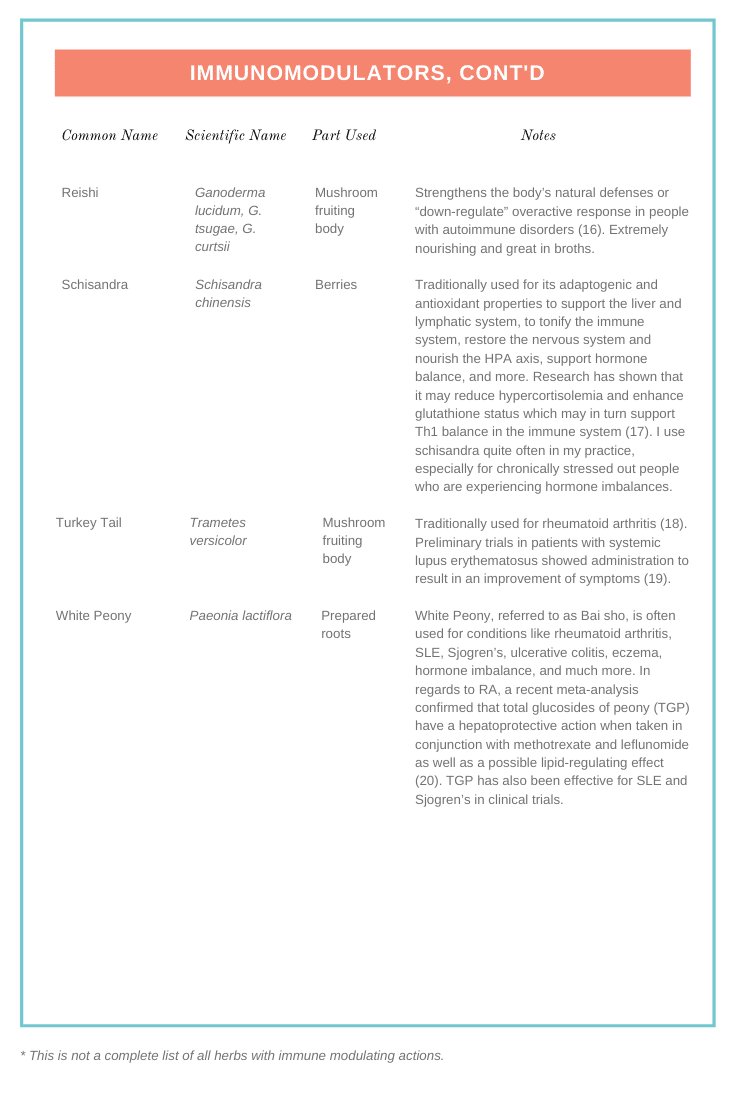
As you can see here, there are so many herbs used both traditionally and by modern herbalists that have the potential to support autoimmune conditions directly. There is so much more to autoimmune herbal intervention than immunostimulants and immunomodulators. Here are some other ways you can look to herbs to support you on your healing path:
Soothing Stress Support. Herbs really shine in their ability to support us through stressful, emotional, and traumatic experiences in our lives – chronic autoimmune illness included. Nervine herbs such as skullcap, lavender, chamomile, wood betony, and linden (among many others) can deeply nourish and soothe our nervous systems in times of heightened stress, during autoimmune flares, or for general day-to-day anxiety.
Digestive System Healing. Herbs may aid in the digestion and assimilation of nutrients, help us to foster more nourishing and emotionally grounded relationships with food, directly support healing intestinal hyperpermeability, and even balance digestive flora and clear things like SIBO. Some of the herbs I often use for digestive system support in clients with autoimmune disease, food intolerances, and GI dysfunction include gentle herbs like peppermint, chamomile, marshmallow root, and plantain leaf.
The list goes on and on.
If you’re feeling called to step on the plant path and learn more about how herbs may support you in your healing journey, I encourage you to start by stepping outside. What plants grow around you? Are there herbs in the garden that can support you right now? Begin by getting to know the plants in your backyard and consider connecting with a clinical herbalist for deeper levels of healing. Just as healing through things the AIP protocol can support our autoimmune wellness journey, so too will fostering connection to our plant allies and cultivating a relationship with the natural world all around us.
References
- Bergner, P. Immunity: Herbal Medicine and the TH1/TH2 Balance. Medical Herbalism 2004:14(2): 1-8
- Waknine-Grinberg, J., El-On, J., Barak, V., Barenholz, Y., & Golenser, J. (2009). The Immunomodulatory Effect of Sambucol on Leishmanial and Malarial Infections. Planta Medica, 75(06), 581-586. doi:10.1055/s-0029-1185357
- Bergner, P. Immunity: Herbal Medicine and the TH1/TH2 Balance. Medical Herbalism 2004:14(2): 1-8
- Lin, B., Cai, B., & Wang, H. (2019). Honeysuckle extract relieves ovalbumin-induced allergic rhinitis by inhibiting AR-induced inflammation and autoimmunity. Bioscience Reports, 39(7). doi:10.1042/bsr20190673
- Dunne-Brady, J., Krueger, T., & Kishnap, S. (Eds.). (2017). Medicinal plants of North America and adjacent herbal regions: Michael Moore (Part 1 – Abies to Crataegus).
- Sun, Y., Jing, Y., Huang, M., Ma, J., Peng, X., Wang, J., . . . Cheng, X. (2019). The PD-1/PD-Ls pathway is up-regulated during the suppression of experimental autoimmune encephalomyelitis treated by Astragalus polysaccharides. Journal of Neuroimmunology, 332, 78-90. doi:10.1016/j.jneuroim.2019.03.019
- Wang, Y., Xie, Q., Liang, C., Zeng, Q., & Dai, Z. (2017). Chinese medicine Ginseng and Astragalus granules ameliorate autoimmune diabetes by upregulating both CD4+FoxP3+ and CD8+CD122+PD1+ regulatory T cells. Oncotarget, 8(36), 60201-60209. doi:10.18632/oncotarget.18732
- Jing, Y., Li, A., Liu, Z., Yang, P., Wei, J., Chen, X., . . . Zhang, C. (2018). Absorption of Codonopsis pilosula Saponins by Coexisting Polysaccharides Alleviates Gut Microbial Dysbiosis with Dextran Sulfate Sodium-Induced Colitis in Model Mice. BioMed Research International, 2018, 1-18. doi:10.1155/2018/1781036
- Chen, J., Yen, J., Lin, C., Tsai, W., Liu, W., Tsai, J., . . . Liu, H. (1993). The Effects of Chinese Herbs on Improving Survival and Inhibiting Anti-ds DNA Antibody Production in Lupus Mice. The American Journal of Chinese Medicine, 21(03n04), 257-262. doi:10.1142/s0192415x93000303
- He, T., Zhao, R., Lu, Y., Li, W., Hou, X., Sun, Y., . . . Chen, L. (2016). Dual-Directional Immunomodulatory Effects of Corbrin Capsule on Autoimmune Thyroid Diseases. Evidence-Based Complementary and Alternative Medicine, 2016, 1-9. doi:10.1155/2016/1360386
- Chen, J., Chen, Y., Yang, S., Ko, Y., & Chen, S. (2009). Immunological alterations in lupus-prone autoimmune (NZB/NZW) F1 mice by mycelia Chinese medicinal fungus Cordyceps sinensis-induced redistributions of peripheral mononuclear T lymphocytes. Clinical and Experimental Medicine, 9(4), 277-284. doi:10.1007/s10238-009-0043-3
- Winston, David and Maimes, Steven. (2007). Adaptogens: Herbs for Strength, Stamina, and Stress Release. Rochester, VT: Healing Arts Press
- Mondal, S., Varma, S., Bamola, V. D., Naik, S. N., Mirdha, B. R., Padhi, M. M., . . . Mahapatra, S. C. (2011). Double-blinded randomized controlled trial for immunomodulatory effects of Tulsi (Ocimum sanctum Linn.) leaf extract on healthy volunteers. Journal of Ethnopharmacology, 136(3), 452-456. doi:10.1016/j.jep.2011.05.012
- Kamyab, A., & Eshraghian, A. (2013). Anti-Inflammatory, Gastrointestinal and Hepatoprotective Effects of Ocimum sanctum Linn: An Ancient Remedy with New Application. Inflammation & Allergy-Drug Targets, 12(6), 378-384. doi:10.2174/1871528112666131125110017
- Guo, A., He, D., Xu, H., Geng, C., & Zhao, J. (2015). Promotion of regulatory T cell induction by immunomodulatory herbal medicine licorice and its two constituents. Scientific Reports, 5(1). doi:10.1038/srep14046
- Winston, David and Maimes, Steven. (2007). Adaptogens: Herbs for Strength, Stamina, and Stress Release. Rochester, VT: Healing Arts Press.
- Bergner, P. Immunity: Herbal Medicine and the TH1/TH2 Balance. Medical Herbalism 2004:14(2): 1-8
- Jin, M., Zhou, W., Jin, C., Jiang, Z., Diao, S., Jin, Z., & Li, G. (2018). Anti-inflammatory activities of the chemical constituents isolated from Trametes versicolor. Natural Product Research, 33(16), 2422-2425. https://doi.org/10.1080/14786419.2018.1446011
- Yarnell, E., & Abascal, K. (2008). Lupus erythematosus and herbal medicine. Alternative and Complementary Therapies, 14(1), 9-12. https://doi.org/10.1089/act.2008.14105
- Huang, Y., Wang, H., Chen, Z., Wang, Y., Qin, K., Huang, Y., … Tu, S. (2019). Efficacy and safety of total glucosides of paeony combined with methotrexate and leflunomide for active rheumatoid arthritis: A meta-analysis. Drug Design, Development and Therapy, 13, 1969-1984. https://doi.org/10.2147/DDDT.S207226













10 comments
Thank you SO much for this post and resource! This fantastic, and information I have been trying to cobble together in past years. Really appreciate it 🙂
Katherine – we think Sarah hit it out of the park on this one. Glad you found it as informative as we did!
I have had testing and have skyrocketing thyroglobulin antibodies, 4040 when the range is 0-40. I am doing a full aip protocol but realize that every morning I have a combination herbal that I make with mostly licorice, hibiscus and echinacea. Could this be the reason I have such wild antibodies? I will stop immediately but just wondering if that is what we are talking about here. Thyroglobulin antibodies. So relieved if this is the problem to have something I can do to help this. I look forward to hearing from you.
Hey Anna! This isn’t my article, but I have Hashimoto’s (autoimmune thyroid disease) and I definitely react poorly to some herbals that are immune stimulants like echinacea and licorice. I am not a medical practitioner and can’t tell you if that is what is going on in your case, but you could be on to something. It would be interesting to talk to your prescribing provider about discontinuing for a bit to see if those antibodies come back into range.
This post lists licorice as an immunomodulator, not a stimulant.
Hi Amy! Thanks for pointing that out. I’ve previously seen licorice listed as a stimulant, and have had clients have similar reactions to Anna above. This is why it is important to consult a qualified herbalist before using herbs especially in supplement form.
Hi Sarah,
Great article! I have Grave’s. Can you send me a full list of herbs that are ok for my autoimmune?
thanks you
Sarah Reyes
Hi Sarah! I don’t think there is a list of herbs that are appropriate for every person with a specific autoimmune disease – skilled herbalists (like Sarah who wrote this excellent article!) evaluate their clients to make custom recommendations based on their history. Sarah is an AIP Certified Coach and her contact info is in her bio, so you should definitely hit her up if you are looking for someone to work with!
[…] Check this article out. These two girls, Mickey, and Angie have done their homework! […]
trust your own body- what?!
some people do not know NOT to drink Echinacea tea because it effects the immune system and people with auto-immune disease SHOULD NOT drink it. It cause the effects of a person with auto-immune diseases to get worse symptoms of their disease